A groundbreaking study has demonstrated that genetically engineered T cells can completely eliminate solid tumors in mice, offering promising potential for treating a wide range of cancers.
Development of Supercharged T Cells
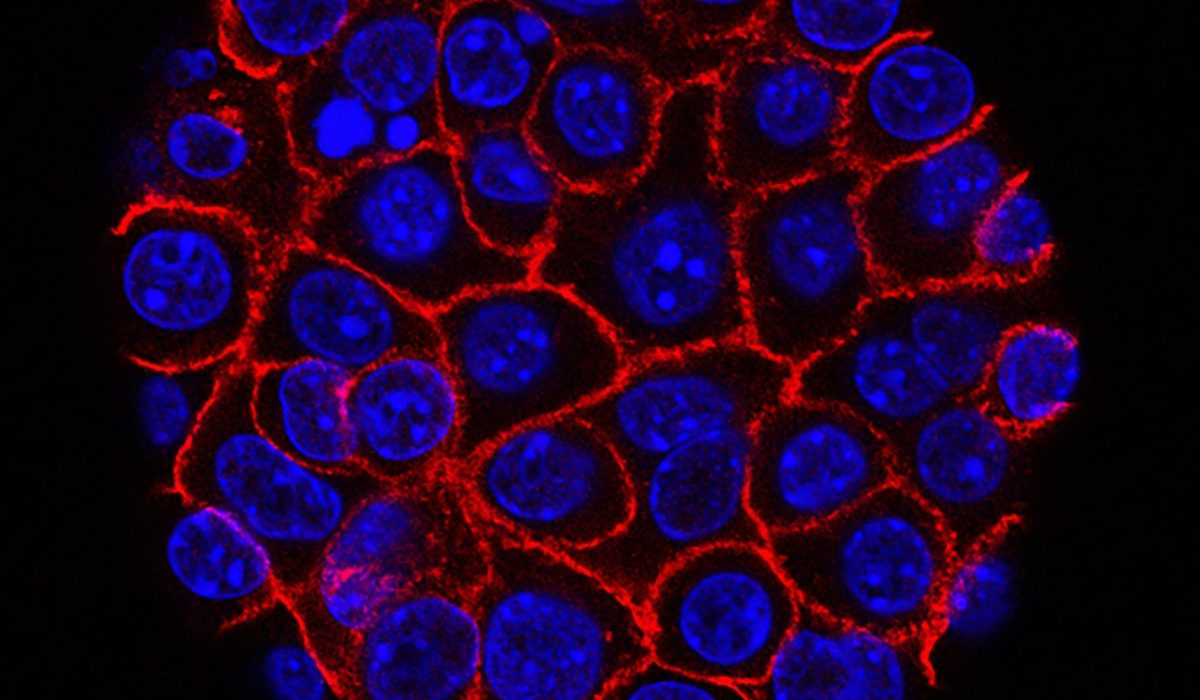
The research focuses on enhancing the immune system’s natural ability to fight cancer. Scientists genetically modified T cells, a type of immune cell, to improve their tumor-targeting and killing capabilities. These engineered cells are designed to recognize specific molecules present on the surface of cancer cells, enabling precise attacks on tumors.
This approach overcomes challenges faced by earlier immunotherapies, which often struggled to penetrate solid tumors or maintain long-term efficacy. The new modification allows T cells to actively seek out multiple solid cancer types, rather than relying on treatments tailored to a single cancer variant.
Effectiveness Against Multiple Solid Cancers
The study revealed that these enhanced T cells were capable of targeting nearly two dozen distinct solid cancer types in the mouse model. In all tested cases, the tumors were entirely eradicated following treatment.
This broad effectiveness marks a significant advance in cancer therapy, as solid tumors have often been more resistant to immunotherapies compared to blood cancers. The researchers noted that this technology holds the potential to become a universal treatment option for numerous hard-to-treat cancers.
Technical Mechanisms Behind Tumor Elimination
The supercharged T cells were engineered to express synthetic receptors that improve their tumor-homing ability and cytotoxic response. These receptors recognize a set of common tumor-associated antigens, ensuring selective targeting without harming normal tissue.
Additionally, the modified T cells exhibit enhanced persistence in the bloodstream and tumor microenvironment, boosting their ability to sustain anti-cancer activity over time. This persistence is crucial for preventing tumor relapse and achieving long-lasting remission in treated subjects.
Implications for Future Cancer Treatments
If translatable to humans, this technology could revolutionize cancer immunotherapy by providing a single treatment modality effective against a wide variety of solid tumors. This contrasts with current therapies that often require patient-specific customization and multiple rounds of treatment.
Clinical trials will be necessary to assess safety and efficacy in human patients, but the preclinical results are encouraging. Success could reduce treatment costs and improve survival rates for many patients with difficult-to-treat solid cancers.
Challenges and Next Steps in Research
While promising, the transition from mouse models to human application entails significant challenges. Human immune systems and tumor biology are more complex, and potential side effects need thorough evaluation. Researchers must also ensure that T cells do not induce harmful autoimmune responses.
The team plans to conduct further preclinical studies to optimize the therapy’s safety profile and explore combination treatments with existing cancer therapies. Progress toward clinical trials will depend on these ongoing efforts and regulatory review processes.