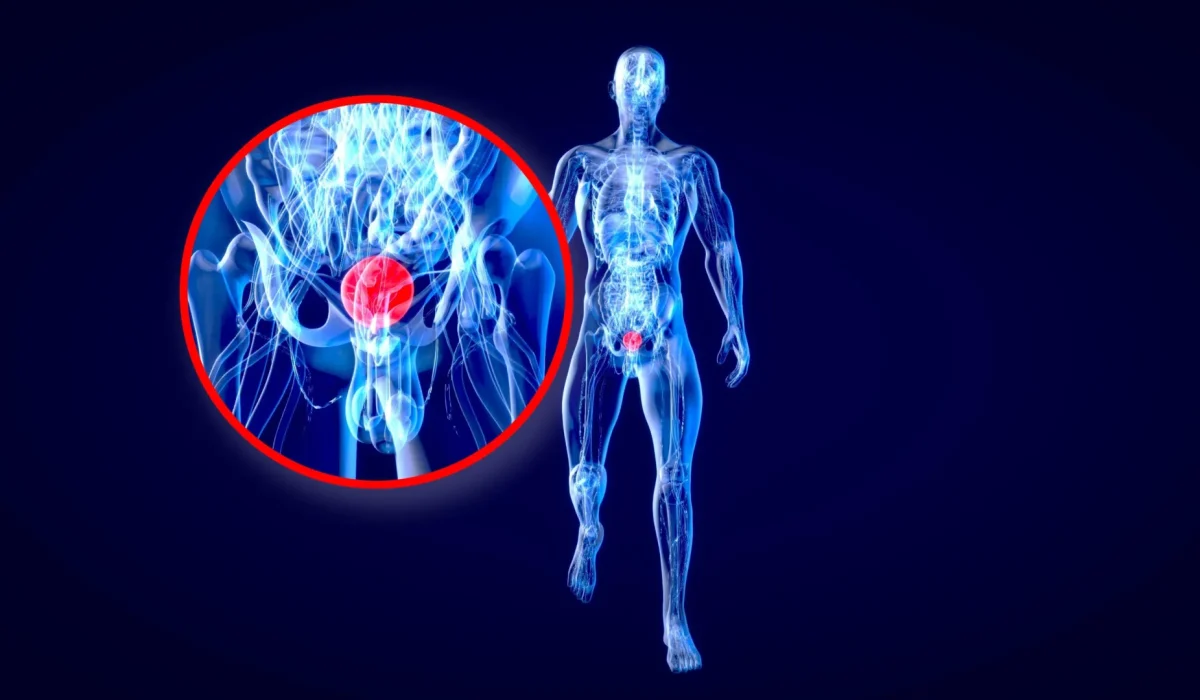
A recent study from Stanford University has revealed that colorblindness could contribute to higher mortality rates among bladder cancer patients. Researchers found that people with color vision deficiency are significantly more likely to have worsened outcomes due to delayed detection of blood in urine, a key early warning sign of bladder cancer.
Study Overview and Key Findings
The research team analyzed millions of medical records over a 20-year period, focusing on patient outcomes for those diagnosed with bladder cancer. They discovered that patients with colorblindness exhibited a 52% higher mortality rate compared to patients with normal color vision. This significant difference highlights a previously underappreciated risk factor related to early cancer detection.
Color vision deficiency, commonly known as colorblindness, makes it difficult for people to discern certain colors. In particular, individuals with red-green colorblindness may struggle to spot red hues, which are important when monitoring for blood in urine.
The Role of Blood in Urine as an Early Warning Sign
Blood in urine, medically termed hematuria, is the most common early symptom of bladder cancer. Prompt recognition of this symptom can lead to earlier diagnosis and improved survival rates. However, for people with color vision deficiencies, detecting reddish discoloration in urine can be challenging.
This difficulty may delay seeking medical advice, thus leading to diagnoses at more advanced stages of cancer, when treatment options are less effective and mortality rates are higher. The study suggests that colorblindness indirectly affects patient outcomes due to this diagnostic hurdle.
Implications for Medical Practice and Patient Awareness
The findings emphasize the need for increased awareness among both healthcare providers and patients with colorblindness. Doctors may consider recommending alternative screening strategies or emphasizing the importance of additional symptoms that accompany bladder cancer.
Healthcare practitioners might also inquire specifically about vision deficiencies during routine checkups to tailor their diagnostic approach. Patient education campaigns could help those with colorblindness recognize that they may be less likely to notice changes in urine color and encourage regular medical evaluation regardless of visible symptoms.
Future Research Directions
Researchers call for further studies to explore potential screening tools adapted for individuals with color vision deficiencies. Technologies such as digital urine analysis or non-visual symptom assessments could help close the diagnostic gap in this patient population.
Additionally, large-scale epidemiological studies may investigate other cancers or diseases where symptom detection relies on color perception, to identify similar risks associated with colorblindness.
Conclusion
This Stanford study sheds light on a novel factor increasing bladder cancer mortality risk—colorblindness—and underscores the importance of tailored approaches in medical screening. By acknowledging and addressing the unique challenges faced by people with color vision deficiency, healthcare providers can improve early cancer detection and patient outcomes.